Stereotactic Radiosurgery: The Revolutionary Advance in the Treatment of Spine Metastases
SCOPE OF THE PROBLEM
In 2016, 1.6 million new cancer diagnoses were made.1 Forty percent of these patients develop metastatic disease to the spine and of those 10% to 20% or roughly 64 to 128 000 develop spinal cord compression.2–4 The risk of a cancer diagnosis increases with age and the segment of the US population older than 65 yr is growing at a faster rate than the general population.5 Targeted therapies, such as biologics and immunomodulators, are being increasingly utilized, but as with cytotoxic agents, are thought to be more effective for visceral and soft tissue disease than bone metastases; thus, despite improved survivals, the expectation is that spine metastases will remain a major source of morbidity. More routine use of magnetic resonance imaging (MRI) and 18F-fluoro-2-deoxy-D-glucose positron emission tomography (18FDG PET) has led to improved detection of spinal metastatic disease. Two-year survival from the time of diagnosis of spinal metastatic disease is 10% to 20%. Taken together, the scope of this problem is greater now than ever before and will likely continue to grow in the future. The goals of treatment for spine metastases are palliative in nature and include maintenance or improvement of neurological function, local tumor control, mechanical stabilization, pain relief, and improvement in quality of life. One major advancement that has impacted, indeed revolutionized, the treatment of spinal metastases over the past 2 decades is stereotactic radiosurgery (SRS). In this article, the authors will review the NOMS (neurological, oncological, mechanical, and systemic) decision-making framework for patients with spinal metastases and the evolution of radiotherapy as a major factor in the paradigm shift driving less aggressive surgery and more radiosurgery in the treatment of this disease. The underlying radiobiology, effectiveness of SRS, and outcome data are also presented.
NOMS
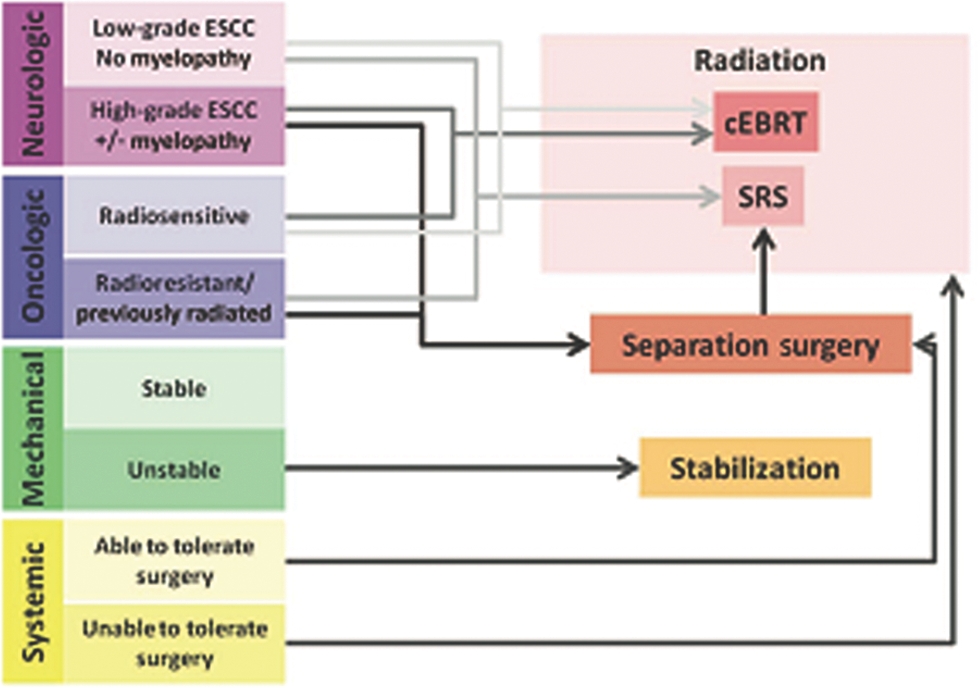
NOMS is a decision-making framework designed to facilitate and guide therapeutic decisions for patients with spinal metastases (Figure 1, NOMS).6,7 It serves as a template for the analysis of important clinical data and as such is not wedded to any particular treatment or technology. As medical science progresses, so too will the treatment modalities utilized within NOMS. Notably, it was conceived for use in a multidisciplinary fashion in conjunction with pain physicians, interventionists, and with input from radiation, medical, and neuro-oncology. The framework is comprised of 4 major domains from which clinical information is assessed: neurological, oncological, mechanical, and systemic.